Pancreas: Conditions and Treatment
What Is the Function of the Pancreas?
What are Common Diseases of the Pancreas?
The pancreas plays a vital role in digestion and metabolic processes. Pancreatic diseases, if not treated, can lead to serious and long-term illnesses.
Some conditions can be treated through medication while others may require pancreatic surgery.
The three most common diseases affecting the pancreas are as follows:
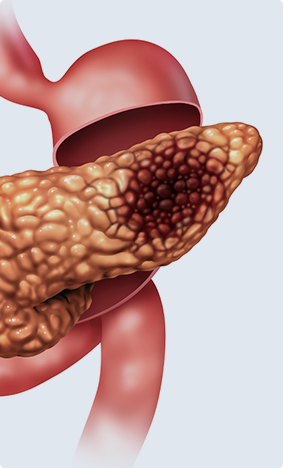
Pancreatitis
Pancreatitis occurs when digestive enzymes that the endocrine tissues produce become prematurely activated while still in the pancreas. This irritates the pancreatic cells, causing the pancreas to become inflamed. Pancreatitis can be acute or chronic, but both have serious consequences if not attended to promptly. Complications include infections, diabetes and kidney failure.
Pancreatitis is typically caused by gallstones that block the common bile duct or in some cases, excessive alcohol intake. It is characterized by severe pain in the abdomen that can extend to the back, nausea and vomiting, bloating, indigestion, diarrhea and fever.
Treatment-wise, pancreatitis often requires hospitalization, antibiotics, pain medication and intravenous (IV) fluids. In cases where pancreatitis is caused by a gallstone obstructing the bile duct, ERCP is necessary. Then, further Gallstones can be removed and prevented by gallbladder removal. Pancreatic surgery in Singapore is sometimes done to drain the pancreas of any dead tissues that have become infected.
Diabetes
Diabetes mellitus is a disorder characterized by a blood sugar level that is too high. It develops when as a result of the pancreas not producing sufficient insulin (type 1 diabetes), or the body being unable to use insulin properly (type 2 diabetes). Insulin is a hormone that transports sugar (glucose) from the blood into the cell, providing them energy to function. With diabetes, there is a lack of insulin, resulting in glucose staying in the blood. This leads to high sugar levels (hyperglycemia).
Diabetes is a serious condition that can have long-lasting or even life-threatening consequences if not treated. These include vision problems, gum disease, kidney failure, heart attack or stroke, nerve damage and loss of limb. Symptoms of diabetes to watch out for are frequent urination, increased thirst and hunger, unexplained weight loss, slow-healing wounds, blurred vision and extreme fatigue.
The first-line treatment for diabetes is insulin, in which insulin is regularly injected into the bloodstream. Other medicines that help stimulate the pancreas to secrete more insulin, and those that prevent the liver from releasing glucose, may be prescribed. In cases where there is pancreas failure, a pancreatic surgeon may recommend a transplant.
Pancreatic Cancer
Pancreatic cancer occurs when abnormal cells develop and multiply in the pancreas, forming tumours. Among the different types of cancer, pancreatic cancer is one of the rarest but also one of the most fatal with a 5-year survival rate of only 20-30%, making prompt detection and treatment even more crucial.
Surgery is the treatment for pancreatic cancer that offers the best chance of long term survival. For cancers in the head of the pancreas, the Whipple procedure (pancreaticoduodenectomy) is performed. The Whipple surgery in Singapore involves the removal of the pancreas head, duodenum, gallbladder, part of the common bile duct and surrounding lymph nodes. Sometimes the pylorus (part of the stomach that connects to the duodenum) is also removed. The remaining organs will then be attached together to help facilitate digestion.
Whipple surgery may be performed via traditional open surgery, laparoscopically (minimally
invasive) or via robotic surgery. The patient may be required to stay in the hospital for
around a week or so. Though laparoscopic and robotic surgery offer reduced risk of
complications and a quicker recovery, they require greater surgical skill to perform. The
Whipple operation is done while the patient is asleep under general anaesthesia.
Whipple surgery is recommended for eligible patients diagnosed with pancreatic cancer and
for removing tumours found in the pancreas. Removing these tumours offer the best chance of
long-term control of all types of pancreatic cancer. After a Whipple operation, most
patients are able to resume normal activities four to six weeks after the operation.
These surgical treatments may be done alongside chemotherapy or radiation therapy. A person can live without a pancreas, though he or she will need to regularly take insulin and other supplements to make up for the function of the lost organ.

Pancreatic Cysts
Pancreatic cystic lesions are being identified with increasing frequency. They range from inflammatory or benign types to precancerous or frankly malignant lesions.
Pancreatic cysts may be classified into inflammatory non-neoplastic pseudocysts or true pancreatic cystic neoplasms (PCNs). Pseudocysts arise on a background of pancreatitis, alcohol abuse, stone disease or abdominal trauma. These lesions are benign and managed based on their symptoms.
The most common PCNs are intraductal papillary mucinous neoplasms (IPMNs), mucinous cystic neoplasms (MCNs) and serous cystadenomas (SCAs). SCAs are benign but IPMNs and MCNs have malignant potential. Other cystic pancreatic lesions make up fewer than 10% of cases and include solid pseudopapillary neoplasms (SPNs), cystic pancreatic neuroendocrine neoplasms (CPENs), cystic degeneration in solid neoplasms and cystic adenocarcinoma of the pancreas.
Pancreatic cysts which have the potential of turning cancerous should be treated by pancreatic surgery with either a Whipple procedure or distal pancreatectomy.

Dr Wong Jen San
Consultant Hepatobiliary & Pancreatic Surgeon
Upon graduating from the University of Leicester and completing his basic surgical training in the United Kingdom, Dr Wong went on to complete advanced training in Singapore before embarking on his HMDP clinical fellowship in Japan—specializing in living donor liver transplantation.
Prior to establishing his own practice, Dr Wong was previously a consultant with the Department of Hepatopancreatobiliary & Transplant Surgery at SGH, an adjunct assistant professor at the Duke-NUS Graduate Medical School and a visiting consultant at the National Cancer Centre Singapore.
Read more
is a Complex and Intricate One

